Polycystic Ovary Syndrome (PCOS) is a common endocrine disorder that affecting millions of women worldwide. Among its many symptoms, acne is one of the most distressing, often impacting self-esteem and quality of life. With other symptoms, it is more challenging to treat when associated with other endocrine disorders.
Address:
Door No. 8-2-293/82/A/725/A, Beside FMS
INTERNATIONAL DENTAL CENTER Road No. 37,
Hitech City Rd, near Daspalla Hotel, CBI Colony,
Jubilee Hills, Hyderabad, Telangana 500033
Email: [email protected]
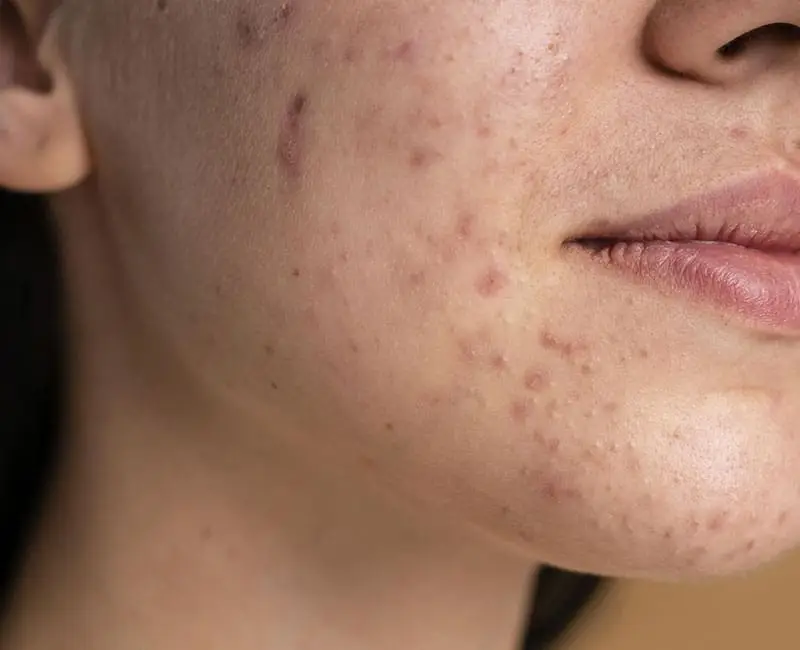
PCOS-related acne is a type of hormonal acne triggered by the hormonal imbalances, which is one the characteristic of Polycystic Ovary Syndrome. PCOS is marked by elevated levels of androgens (male hormones) and insulin resistance, which can lead to various symptoms, including irregular menstrual cycles, excessive hair growth, weight gain, and persistent acne. Unlike adolescent acne, which typically resolves with age, PCOS-related acne usually persist from teenage into adulthood and is often more challenging and difficult to treat.
Symptoms of PCOS-Related Acne
PCOS-related acne can present in various forms and typically manifests in the following ways:
Persistent Pimples and Cysts: These are inflamed, red, and sometimes painful lesions that can appear anywhere on the face but most commonly seen along the lower cheeks, jawline, chin, and upper neck. They can also appear on the chest and back.
Comedonal Acne: This includes blackheads and whiteheads, which are non-inflammatory lesions present mainly on T zone area of face, that can become inflamed if not treated properly.
Severe Breakouts: These can be more severe and long-lasting than typical acne, often resistant to standard over-the-counter treatments.
Scarring: Due to the persistent and often severe nature of the acne, scarring can be a common outcome, leading to pitted or raised scars on the skin, thereby damaging the skin.
Causes of PCOS-Related Acne
Several factors contribute to the development of acne in women with PCOS:
Effectively managing PCOS-related acne requires addressing both the skin symptoms and the underlying hormonal imbalances. FMS Skin and Hair Clinics provides the most effective treatment options.
Hormonal Treatments:
Topical Treatments:
Oral Medications:
Low-Glycemic Diet: Reducing the intake of high-glycemic foods (like sugary snacks and refined carbohydrates) can help manage insulin levels and reduce acne.
Anti-Inflammatory Diet: Incorporating foods rich in omega-3 fatty acids (like fish, nuts, and seeds), antioxidants (like fruits and vegetables), and whole grains can help reduce inflammation and improve skin health.
Regular Exercise: Physical activity can improve insulin sensitivity, reduce stress, and promote overall hormonal balance.
Skincare Routine:
Gentle Cleansing: Use a mild cleanser twice daily to remove excess oil and impurities without irritating the skin.
Non-comedogenic Products: Choose skincare and makeup products that do not clog pores.
Moisturizing: Even oily skin needs hydration. Use a lightweight, non-comedogenic moisturizer.
Sun Protection: Application of a broad-spectrum sunscreen with an minimum SPF of 30 or higher daily to protect against UV damage, which can exacerbate acne.
While treating existing acne is crucial, preventive measures can help reduce the frequency and severity of breakouts:
Manage Stress: Engage in stress-reducing activities such as yoga, meditation, and adequate sleep to help balance hormones.
Healthy Diet: Maintain a balanced diet rich in fruits and vegetables which are rich in omega 3 fatty acids, whole grains, and lean proteins. Limiting intake of refined sugars and dairy products can help manage insulin levels and reduce acne.
Regular Skincare: Establish and maintain a consistent skincare routine. Cleanse, exfoliate, and moisturize regularly, and use treatments as recommended by a dermatologist.
Avoid Touching Your Face: Keep hands away from your face to prevent the transfer of dirt and bacteria.
Clean Bedding and Towels: Change pillowcases and towels frequently to reduce the risk of bacteria and oil transfer to the skin.
Stay Hydrated: Drink plenty of water to keep the skin hydrated and flush out toxins.
When to See a Dermatologist
If over-the-counter treatments and lifestyle changes don’t improve your acne, or if your acne is severe and causing scarring, It is essential to consult best dermatologist. A professional can assess your skin, diagnose any underlying conditions, and create a tailored treatment plan. This may include prescription medications, professional treatments, or a combination of both to effectively manage your acne.
PCOS-related acne can be a persistent and distressing issue, but with the right knowledge and treatment approach, it is manageable. Understanding the hormonal imbalances that drive PCOS and exploring various treatment options can help you develop a skincare regimen that works for your unique skin type and needs. By incorporating preventive measures into your daily routine, you can reduce the likelihood of breakouts and maintain clear, healthy skin. With patience and consistency, you can overcome PCOS-related acne and enjoy a complexion that radiates confidence and vitality.
Email: [email protected]